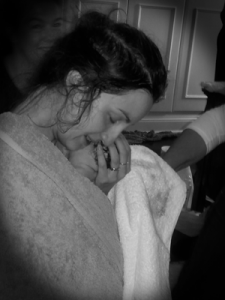
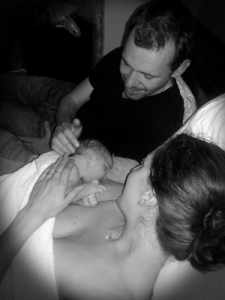
Our little breechling
By Ali Barker
We planned a home water birth for the birth of our first baby. We had bought a pool which we blew up at the weekend I turned 40 weeks pregnant (10 August 2014) and felt ready for labour to commence. However a few issues presented themselves at the latter stages of my pregnancy which had a great bearing on the planned birth.
During a routine ante natal check carried out at our home when I was 40 weeks + 1 day on 18 August 2014, a midwife, whom I had not seen previously, carried out palpation on my bump and suspected our baby may be breech. I could not believe it. All previous ante natal checks had identified our baby (given the moniker, Beatty) as head-down and, by this stage, 4/5 engaged. I was shocked to hear this at this late stage in my pregnancy.
The midwife was fairly confident that our baby was head-down. Such was her conviction, she sent me for a scan at the hospital the following day, rather than an emergency scan on the same day. Upon arriving at the hospital, the midwife carried out palpation and she also thought the baby was head down. However, upon carrying out the ultrasound scan, one of our biggest fears was realised when our baby was confirmed as being breech. I was devastated as I believed our home birth was an impossibility and I was naturally concerned as to any consequences of the breech presentation in relation to our baby’s health/delivery.
I had to wait in the hospital from 11am on Tuesday 12 August 2014, when the breech was diagnosed, until 7.30pm, before an ECV (a procedure carried out by a consultant doctor to try and manually turn our baby) was performed. I was told this was because I needed to be nil by mouth in the event I needed to go into theatre for an emergency C section. This was far from ideal at 40+ weeks pregnant on a hot summer’s day on a hospital ward. After the ECV failed to turn Beatty, I was told by the NHS that the only option was a C section.
While I waited for the ECV procedure to be performed, I started to research breech birth and came across midwives who were experienced in the field. From my research, it seemed that breech presentation was not abnormal, it was, in fact, a variation of normal. This was something I held at the forefront of my mind in the coming days.
As I was 40 weeks + 2 days, the hospital wanted me to sign a consent form to have a C section on Friday 15 August 2014. I asked the hospital whether it was possible to deliver a breech baby vaginally but I was told this skill was a “dying art” amongst midwives.
I spent that evening/into the early hours of the next day frantically researching breech presentation and the possibility of vaginal breech delivery. The possibility of a breech vaginal delivery was not discussed at the hospital.
I had been practicing Natal Hypnotherapy for the majority of my pregnancy and attended a 2 day workshop in Wimbledon. This, I believe, gave me the confidence to trust my body’s ability to give birth naturally and to trust my instincts, both of which led to our birth story I describe below.
On the evening of 12 August, after I was discharged from hospital, I searched Google for “natal hypnotherapy” and “vaginal breech” and found Ruth Atkinson’s birth story. I emailed Ruth at an ungodly hour desperately hoping she would reply to my email. Time really was of the essence given the late stage of my pregnancy. I was truly grateful when I saw Ruth’s reply in my inbox at around 11pm at night. One of the things she said which gave me an element of hope was “All is not lost. It is still possible to have the birth you want…”
Ruth kindly spoke to me the following day and shared her birth story which was, strangely, not too dissimilar to mine in respect of the breech diagnosis late in her pregnancy and her desire to have a vaginal breech delivery. Ruth told me about the wonderful independent midwives who had supported the safe arrival of her breech daughter, vaginally, at home.
I wasted no time and contacted the same independent midwives who then came to our house the following day to discuss matters in person. My husband and I digested all of the information and decided we would engage their services. I was so happy to have their assistance as they shared similar views to my husband and I as to natural birth.
This sentiments of this quote rang true during this time:
“The more Wisdom you attain and the more Conscious you become, the crazier you will appear to others”
I think Beatty knew not to come until we had our team in place. By this time, we had an excellent, supportive team together (including my wonderful husband). It was therefore a matter of waiting for labour to commence.
By 41 weeks, Beatty had still not arrived. However, the midwives recommended that I ought not to do anything to try and augment labour, whether that be reflexology, acupuncture and/or a membrane sweep as it was important for a breech baby to come when it was ready, or opt for C section. So, it was a matter of (patiently) waiting.
Our independent midwives therefore embarked on ‘Project Relaxation’ as it seemed apparent that my body/mind were in a state of flux given the issues of the preceding week. I believed that I would not go into spontaneous labour until I switched of my ‘thinking brain’ and allowed my primal bran to engage, something I learnt in Natal Hypnotherapy.
All the while, I was getting many messages from friends/family wondering if we had had our baby. As each day went by, I was getting more anxious as I knew post 42 weeks would bring further issues to bear. We had even booked a fetal well being scan on Harley Street (as we were keen to avoid attending the hospital, where possible, to avoid further pressure from the hospital as to an elective C section) to check Beatty’s heart beat, amniotic fluid and blood flow to the placenta.
I was not overly concerned as there is perhaps unnecessary significance placed on the ‘guess date’; many people had said to me that babies come when they are ready. In France, for instance, full term is considered to be 41 weeks, so there are different interpretations of ‘full term’. Beatty continued to be very active with lots of kicks which the independent midwive said was a good indicator of Beatty’s wellbeing.
I wrote a letter to Beatty and read it aloud to her and also talked to Beatty several times a day to try and encourage her to start her journey into the world. I knew we could do it together and I truly believed that.
At 41 + 6 days, my contractions started at 3.45pm on 23 August 2014, while eating strawberries and cream in the garden on a lovely warm day. They were irregular and not very strong. I had had the same sensation a couple of days before, while watching a DVD, when I had to get out of bed to ease the sensation, however on this occasion it passed after an hour or so. We were therefore convinced that this was another false start. Nevertheless, we walked to the park to try and encourage more contractions. While I had a few sensations, they continued to be irregular and did not increase in intensity. We did, however, practice filling the pool but promptly emptied it, again not anticipating labour to commence imminently.
We received a message from one of our NCT group at around 2.30pm that day to confirm they had welcomed their little boy into the world, 2 days’ early. I was delighted for them but it served to emphasise the fact we were still waiting for our little one.
After a little break from the contractions, we retired to bed. However, by 8.30pm the contractions were coming more frequently and with increased intensity. We therefore called our independent midwives to come to the house.
My surges were concentrated in my back so my husband massaged my back with increasing force to counteract the sensations. My contractions continued but did not seem to progress sufficiently therefore the midwives retired to bed. I continued to have infrequent contractions throughout the night. I recall shouting at my husband (who was asleep) to massage my back throughout the night. We all woke up around 7am and, as my surges continued in a similar manner, the midwives decided they would give my husband and I privacy to seek to encourage labour to progress. They all went into the local town for breakfast.
My husband made me breakfast of yoghurt and fresh fruit but I promptly threw this back up again. I was in the kitchen on my exercise ball and could feel myself drifting away from my husband and the environment around me and retreating into my own body. Once the midwives arrived back at 8.30am, I was in established labour. The midwives did not carry out any internal vaginal examinations, rather they read my behaviour to assess progress.
I had never really considered where I would labour in the house but I remained in the bedroom. I recall it was a lovely sunny day outside but we kept the curtains closed to create a more ‘safe’ enclosed environment. The Natal Hypnotherapy relaxation music was playing in the background for the duration of the labour and we had lavender essential oil in a diffuser. The midwives were very respectful of our own space and left my husband and I alone for much of the time.
My waters broke in our bathroom during one of my contractions at around midday. I realised I was getting ever closer to meeting our baby!
My husband and I were prepared for the transition stage from labour to pushing. However, I do not recall this period in the labour, nor does my husband; although, in retrospect, it may have occurred when I asked the midwife if I could use gas and air. I think this was a moment of slight panic in my mind when I knew I was entering the final stage and thought I may need assistance. The midwife gently discouraged this and I was happy to proceed without gas and air. I did have 2 paracetamol at some stage but not sure they would have had any effect whatsoever!! I did, however, use my TENS machine throughout labour and found this really helpful for easing the effects of the surges and it also served as a distraction, together with the tools I learnt with Natal Hypnotherapy. I also made loud chanting sounds of AHHHHH and OOOOOM to get through the surges which I learnt from JuJu Sindin’s Birth Skills book – I would highly recommend this.
At around 3pm ish we were all preparing for the birth of our daughter. The midwives prepared the bedroom with the dust sheets and old bedding. I assumed a side lying position on my left side. This was an odd position in the sense that I had never considered this position in any of my birth preparation classes.
I recall the bedroom was very hot as we had to use a heater to ensure the room was sufficiently warm to receive Beatty. During the pushing stage, my husband cooled my forehead with a cold flannel which was replaced regularly by the midwives to ensure it was cool. I also had lots of coconut water throughout the labour, together with ice cubes, made of honey/lemon and himalayan sea salt, raspberry leaf infused water and black molasses in hot water to maintain my energy levels.
Beatty was slowly descending but I could sense that the midwives were keen for me to change positions, although they very much allowed this to be led by me. As a matter of common sense, it would have been more logical for me to be in a vertical position/all fours. I had pulled a muscle/ligament on my left side at some stage during labour so I was not desperate to change positions, as I knew it would hurt. However, something urged me to jump onto an all fours position. Once I changed position, Beatty seemed to descend much quicker.
The midwives have since commented on the extent of my movements during this stage – I was almost kneeling at one point, then swaying my hips left to right and then leaning forwards in a prayer position. All of this behaviour was instinctive, rather than conscious, and the midwives believed this assisted our daughter’s birth. It felt like Beatty and I were doing a little dance with one another. I was comforted that our daughter was almost dancing with her little legs hanging out of me and she was a lovely colour, whereas some of the videos I had seen of vaginal breech deliveries involved a baby looking a little limp and blue.
I recall the sensation of our daughter’s bum coming out and then her legs. I could sense when Beatty’s body had flopped out. I recall looking through my legs and seeing Beatty hanging there, with her head inside of me. We had kept the sex of our baby a surprise so I was constantly asking the midwives if they could discern the sex. As our baby passed urine, they could tell it was a girl. My husband and I were so surprised as 95% of people had said they thought it was a boy. While we had no firm view either way, we had become convinced that it was a boy; it was a lovely surprise to hear it was a girl.
I did not have another contraction to push out Beatty’s head for around 5 minutes. It felt like a long time. The midwives were not too concerned as our daughter’s lips were peeping out of me and her lips were opening and closing to take in air. The only time the midwives intervened was to lightly move the cord to allow our daughter to breathe safely.
As no contraction came, I pushed without a contraction and my daughter was born at 4:17pm, exactly 14 days after her due date. It was the best feeling. My husband, who had been attending to me the whole labour, gave me a big kiss and then the midwives put our daughter in front of me on the floor. I couldn’t believe she was ours. I didn’t pick her up straight away while I took it all in. I then held her close to my chest – skin to skin – and we had our first cuddle as a family.
Our daughter was 8 lbs 9 ounces (the midwives did comment on how big she appeared as she was being born – I always had a strong suspicion that she was going to be a big baby!) and 52 cm long – although she appeared much longer; most people have passed comment on this since her birth. Our daughter scored 9/10 on her APGAR score.
Given established labour started around 8.30am that morning, labour was fairly quick. I also only suffered a minor tear which did not require any stitches. When I spoke to a midwife before the birth she told me that breech births are generally fairly quick and that generally women don’t tear – so breech birth does have its advantages!
We then all moved to our bed with our daughter in my arms while the midwives tidied up around us. One big bonus was that the student midwife used to be a chef so she made an amazing breakfast for us of eggs, bacon, spinach and tomatoes – beats hospital food any day!
One of the midwives also made me a lovely placenta smoothie and I ate some of the placenta immediately after the birth, when resting in bed. I cannot be certain, but I attribute the fact that I did not suffer any baby blues to the placenta which I consumed. I believe this regulated my hormones and replenished vital nutrients lost during labour.
I will treasure forever the memory of the three of us snuggling in bed that evening. If we had given birth in the hospital, my husband may have been asked to leave us that evening which would have been awful. This was another (of many) advantages to a home birth.
 Our daughter was slow to latch on but after a couple of days of practice, she was guzzling away – her new found hobby.
Our daughter was slow to latch on but after a couple of days of practice, she was guzzling away – her new found hobby.
If the hospital had had its way, our daughter would have been born on 15 August 2014; that was not her time. In fact, the midwives noted that our daughter did not show any signs of being particularly over her due date. We were delighted she came naturally on her true birthday and not a date fixed by a hospital.
We did not name our daughter until a couple of days after the birth; such was our belief that our baby was a boy, we had not properly considered girls’ names. On Tuesday 26 August, we named our little breechling Estelle Augusta Barker – inspired by the main character in Charles Dickens’ novel, Great Expectations, Estella. A strong, formidable character which we hope Estelle will be, too.
BIO
Ali Barker gave birth with the assistance of Maya Midwives, Kathryn Weymouth, Liz Nightingale and Suyai Stenhauer. Ali is married to Sam Barker and they are looking forward to celebrating 10 years together this summer 2015. They are very much still in love and have enjoyed every single moment spent with their breechling, Estelle.